How Can Participating in a Clinical Trial Help Me? (A Focus on CIDP)
Research & Clinical Trials
Read on to learn more about the basics of clinical research & why it is important to participate. Alternatively, click here to learn more about the ongoing clinical trials currently recruiting participants.
The Research Process: Bench to Bedside
The practice of medicine and treating patients involves a great deal of work “behind the scenes”. Many doctors, biologists, chemists, pharmacists, and other researchers dedicate their ideas, knowledge, and expertise to study potential new treatment options to treat, and possibly cure, medical conditions. This usually takes years, sometimes decades, and plenty of funding. Before a potential new treatment moves into the clinical trial phase, where it is given to human patients, the safety profile of the potential new treatment is studied extensively in the lab and often tested in animal models. This way, patients that take part in clinical trials can be assured that only the best, and most safe, potential new treatments make it to the clinical trial phase.
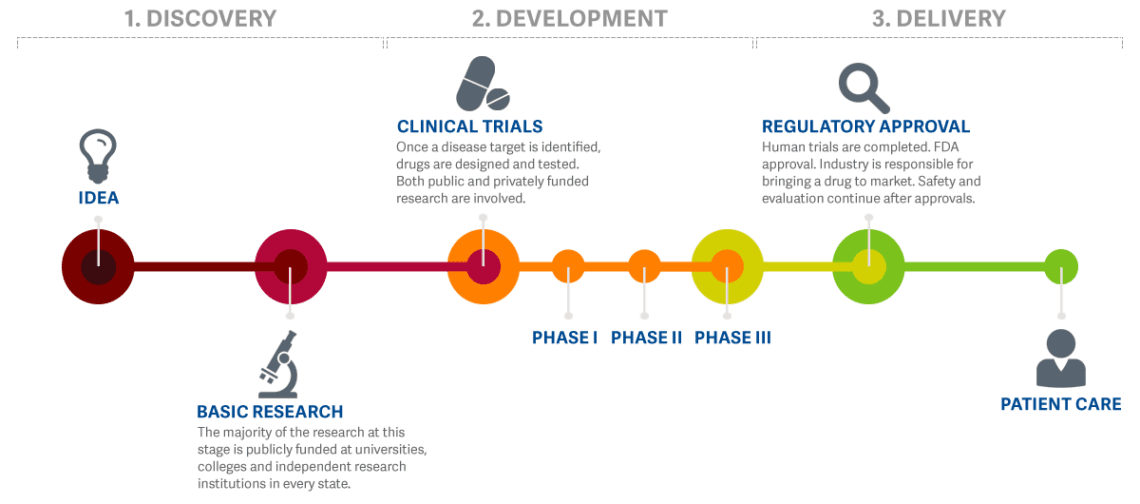
Before Clinical Trials in humans can start, investigators must submit all the data generated in the laboratory and in animals, for review by the scientists at FDA, to see whether there is any indication that this treatment might potentially be harmful. Investigators must also share some manufacturing details and characterization of the new chemical entity proposed to be tested in humans. The FDA must either request additional information from the investigator within 30 days or allow the clinical trials to begin.
Clinical Trial FAQs
Topics
If you are interested in a clinical trial, you should always first discuss this decision with your doctor; there is a chance your current doctor is part of the clinical trial team. If they are not, they will still be your doctor and will be in charge of overseeing your care. However, you will likely have to visit a doctor who is part of the clinical trial team in addition to your regular doctor.
Every clinical trial will have different requirements, but most clinical trials include a schedule of regular visits with doctors and nurses on the study team within a relatively short time-frame.
- Site: The hospital or medical center where a clinical trial is taking place. Clinical trials often have many sites across a country or many countries.
- Investigator: The doctor leading the clinical trial team at a particular site.
- Sponsor: The entity – possibly a drug-maker or government agency – that is responsible for creating and overseeing the clinical trial.
- Investigational drug / experimental drug / investigational product: The potential product, not yet approved for marketing for a specific disease, that is being tested in a clinical trial. It can be a drug, a blood or plasma product, a medical device, or a medical procedure/technique.
- Placebo – A placebo is sometimes referred to as a “sugar pill”, but can be any number of treatments that are not the potential new treatment being studied. In order to test the effectiveness of a drug, researchers need to determine the effectiveness of a potential new treatment, researchers compare the disease course and symptoms when the potential new treatment is taken vs. when it is not. When someone is not taking the potential new treatment during the clinical trial, they are taking the placebo.
- Placebo vs. control: Placebo does not always mean “sugar pill” or “no treatment given”. Sometimes, clinical trials test new potential treatments against what is the current standard of care. If someone is not getting the potential new treatment, they are acting as the “Control” in the clinical trial. In some innovative trials, people act as their own control, meaning they go through a period in the trial where they take the potential new treatment and compare their symptoms to a period when the person did not take the potential new treatment.
- Blinded: During a clinical trial, results are more valid if researchers are able to compare how symptoms change in patients taking the potential new treatment against those who do not when the researchers do not know who is receiving which treatment. This helps to eliminate bias (everybody wants new treatments to work!). People that might be blinded in a clinical trial include the investigator (doctor), the clinical trial team, the patient, the researchers doing the data, and the study sponsors.
- How will the study team communicate with my regular doctor?
- Will the study sponsor cover any expenses not covered by insurance? Is there an opportunity to be reimbursed for traveling to participate in the trial?
- What is the plan for care or receiving the drug when the trial is over?
- When will I know whether I received the potential new treatment being studied in the trial?
[Answer given by Dr. Sami Khella, Professor and Chair of Neurology, Penn Presbyterian] When a new medicine is tested in a clinical trial, frequently, a patient participating in the trial will be asked to stop her or his current medicine usually for a short period of time. This is called “a wash out period” or “a run-in period.” As the name wash out implies, it is done for 2 reasons:
- To clear the medicine itself from your body, and to clear its most recent effects on your body. This gives the new medicine a chance to work without confusion from the effects of the old medicine.
- To avoid a drug-drug interaction between the old and new medicines.
Remember that participants in clinical trials are monitored very closely and the health and safety of all participants is the top priority of any clinical trial.
GBS|CIDP Specific FAQs
Topics
While it is likely that our Centers of Excellence participate in cutting-edge research, these centers are not exclusive to GBS|CIDP research. Therefore, clinical trials may also be taking place at other hospitals/doctor’s offices, so please talk to your doctor and the clinical trial team to learn more.
Ongoing Clinical Trials
There are several clinical trials in process right now that support research for GBS, CIDP, and variants. Please note that this information is intended to help patients be aware of all of their options; the Foundation is unable to endorse any clinical trials.
Clinical Trials for People Currently Experiencing GBS
Topics
A Phase 1b Study to Evaluate the Safety, Tolerability and Drug-Drug Interactions of ANX005 and Intravenous Immunoglobulin (IVIg) in Subjects With Guillain Barré Syndrome
The international GBS Outcome Study (IGOS) is the largest and longest prospective trial designed to collect extensive data from patients afflicted with GBS in a systematic manner. The aim is to collect information from patients by intensive international collaboration. All patients are followed at standard intervals from the earliest phase of the disease up to at least one year after. At these time points all patients are clinically examined and documented according to the same protocol. The data generated from IGOS may fundamentally change how we care for patients with GBS and hasten research for more effective therapies.
The GBS|CIDP Foundation International is currently funding the IGOS trial through a research grant.
Clinical Trials for People Living with CIDP
Topics
This biomarker study will collect blood samples before and after IVIg treatment from people with CIDP diagnosed and followed at GBS|CIDP Foundation International Center of Excellence (COE) clinics. A network of mobile medical professionals will schedule 4 blood collection visits at the participant’s home over the course of approximately one month. The study goal is to better understand how circulating biomarkers change in response to IVIg treatment in people with CIDP with the aim of incorporating biomarkers into future interventional clinical trials.
This is a Phase 2 study to evaluate the safety and efficacy of the subcutaneous formulation of efgartigimod in adults with CIDP.
CSL Behring is conducting an open-label study to investigate the efficacy of single and multiple-dose Privigen administration in IVIG‑pretreated and IVIG-untreated pediatric subjects with chronic inflammatory demyelinating polyneuropathy (CIDP).
ClinicalTrials.gov Identifier: NCT03684018
ADVANCE CIDP 1 Clinical Study
CIDP Treatment Trial, Now Enrolling Patients Worldwide!
Announcing a new study to investigate a potential new medication for CIDP patients. The ADVANCE-CIDPTM 1 Study is looking at a potential new treatment (an investigational medication) for patients with chronic inflammatory demyelinating polyradiculoneuropathy (CIDP). It will assess if the investigational medication could help to prevent muscle weakness in the upper and lower limbs. The investigational medication is an immunoglobulin (made from proteins found in the body called antibodies) and is given as an infusion under the skin every 2, 3, or 4 weeks.
About the study
The study is currently looking for 170 patients at approximately 90 study centers worldwide.
If you take part, you may be involved in the study for up to 14 months. The study is now enrolling. Requirements include:
- Must be 18 years of age or older
- Must have been diagnosed with CIDP
- Must have been receiving treatment with immunoglobulin infusions at a stable dose, every 2–6 weeks, for at least 12 weeks (3 months)
Please visit clinicaltrials.gov and search for study identifier NCT02955355 for more information, including a list of participating countries and study centers:
Clinical research studies are scientific evaluations in people, led by researchers and physicians. They can help advance the understanding of a disease and are the most important way for researchers to find out if potential new treatments are safe and effective. Studies like these are needed to be able to make new treatments available to patients.
